What’s causing the E. coli outbreak in four U.S. states?
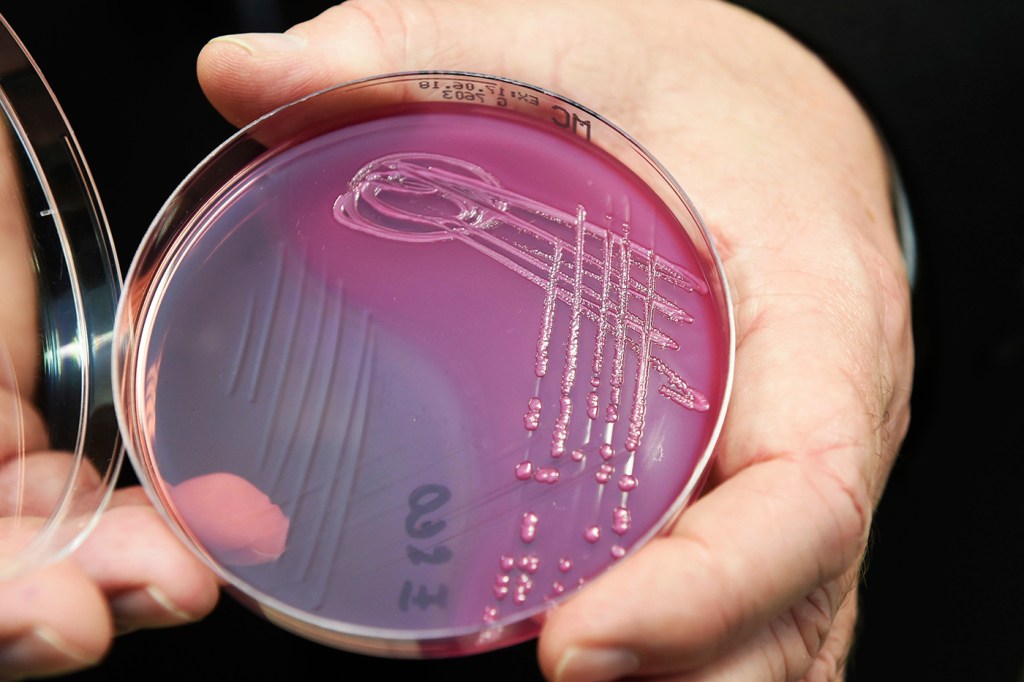
An E. coli outbreak in the Midwest has public health officials scrambling to discover the source.
Thirty-seven infections have been reported in Michigan, Indiana, Pennsylvania and Ohio, including 10 hospitalizations, the Centers for Disease Control and Prevention reported this week.
According to the CDC, symptoms of E. coli poisoning start within three to four days of exposure, and include stomach cramps, diarrhea and vomiting, and many infected individuals will recover without going to the hospital. But there is one gap in officials’ knowledge about the current outbreak—they don’t know what caused it, though lettuce from Wendy’s sandwiches is currently a suspect, the New York Times reports.
“That is hopefully going to change rather quickly,” says Darin Detwiler, assistant dean of academic and faculty affairs at Northeastern University’s College of Professional Studies in Boston. “But it takes a lot of work.”

According to Detwiler, the first big E. coli outbreak was in the 1980s, and in 1993, a severe outbreak affected hundreds of people and killed four children, including Detwiler’s 16-month-old son. The number of deaths attributed to foodborne illness in the United States has remained pretty steady since then, with about 3,000 Americans dying each year. This year’s spike in the Midwest is more egregious than usual, however.
And it’s likely worse than we know. In the CDC’s report, the organization notes that “the true number of sick people in this outbreak is likely higher.” That is likely because those who have severe and prolonged symptoms—which include diarrhea, bloody stool and decreased urine output—are more likely to go to the hospital and therefore have their case reported to public health authorities, Detwiler says. The very young, the elderly, pregnant people, and the immunocompromised are more likely to fall into this category.
But most of those infected will experience no symptoms or mild to moderate ones, and won’t bother going to the hospital. Incidentally, if you ever uttered the phrase, “It must be something I ate,” it’s likely you had E. coli, Detwiler says. For every foodborne illness case that is reported, he says, up to 22 are unreported, according to some estimates.
This means less data to discover the source and prevent more people from getting sick.
This process can already take time and lots of “detective work,” says Mansoor Amiji, distinguished professor at Northeastern’s Bouvé College of Health Sciences. It involves charting the movements and eating habits of the 29 people in the three to four days before they became sick and finding a commonality. Maybe they all ate at the same restaurant or event, or maybe they all swam in the same pool, or went to the same petting zoo—the latter two of which can be contaminated with E. coli.
Lab work can confirm whether all 29 of the cases are from the same E. coli strain, meaning the infection likely came from the same source. This testing works similar to how samples are tested for COVID-19, Amiji says. When a sample is sent to a lab, nucleic acids are extracted and compared to another strain, being careful to differentiate it from the E. coli that exists naturally in the human body.
Once a source of infection is identified, testing can confirm if it matches the cases as well. All in all, the time between initial infection and the determination that it is part of a known outbreak can be three to four weeks, according to the CDC.
Unfortunately, lab work cannot help narrow down the source—E. coli in meat, for example, doesn’t necessarily look different from E. coli in water, Amiji says. Another complication is that E. coli can pass from person to person. And when there is no one event that caused the outbreak—for example, if a food truck spread E. coli around town for a day—it can be particularly difficult to pin down a source.
In this case, where a big spike in infections happened in a relatively short period of time, it may actually make it easier to discover the source, as it indicates an event or a particular restaurant, Detwiler says. Meanwhile, cases trickling in more slowly can make the detective work more difficult, though in general, the more data points, the better.
Does this mean you should report to your doctor every time you have a stomach bug? It likely won’t make a difference when it comes to outbreaks, Detwiler says, and you may not even have enough of the bacteria to show up positive in test results.
Or, you may not even be tested at all. According to Brandon Dionne, associate clinical professor at Northeastern’s Bouvé College of Health Sciences, testing is usually done for people in high-risk groups and for those with severe symptoms, like a fever above 102. However, “if there is a known outbreak, clinicians might also be more likely to suspect the disease and may be more likely to test for it,” he says.
While there isn’t a strict threshold of symptoms to test positive for E. coli, more severe symptoms generally mean more of the bacteria is present, though stronger PCR tests can detect smaller amounts.
This means reporting your everyday stomach bug isn’t likely to provide helpful information. What is helpful, Detwiler says, is reporting to officials if you get sick as part of a known outbreak. If public health officials report that there was an outbreak at Boston Calling, and you became sick after attending the festival, then reporting is helpful in order to create more data points, along with information about where you went and what you ate.
“That’s going to help them in terms of those numbers,” he says.
For media inquiries, please contact media@northeastern.edu.






