Omicron has set records. How much do case counts matter now?
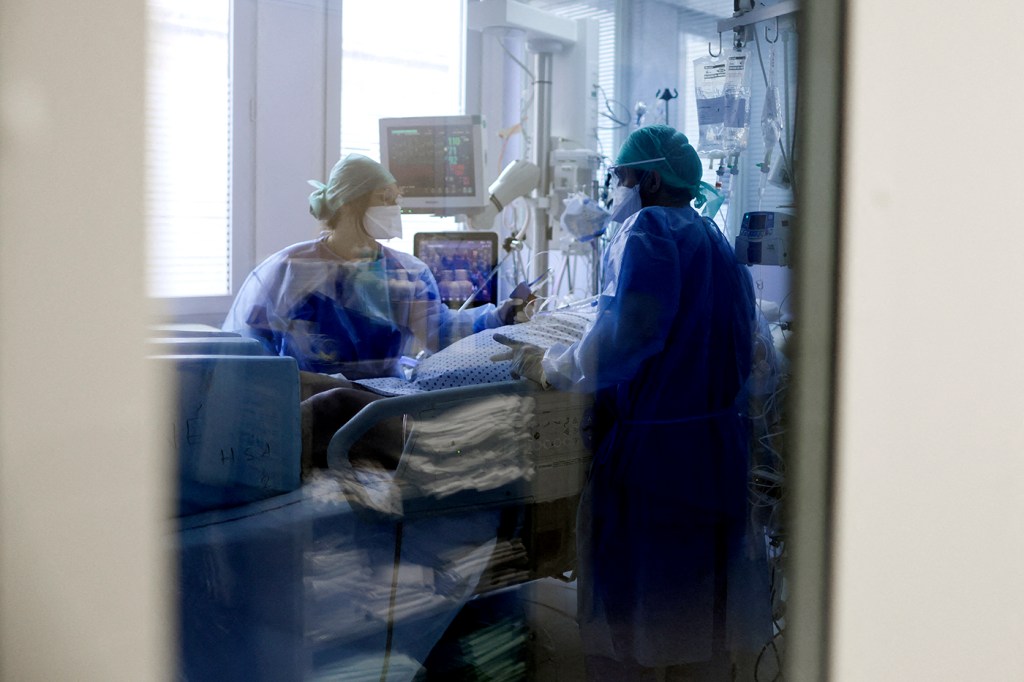
Despite the overwhelming numbers in the current wave of COVID-19 cases, Northeastern experts say we have not been set back to March 2020. In 2022, the pandemic is different.
The omicron-fueled surge has set and reset daily COVID-19 case count records several times. And this week, the U.S. set a new record for pandemic hospitalizations, with 145,982 COVID-19 patients occupying hospital beds as of Tuesday. The previous record was set last January at 142,315, according to The New York Times. These totals also include people who were admitted to the hospital for other conditions and then incidentally tested positive for COVID-19.
But nearly two years into the pandemic, high numbers shouldn’t prompt the same panic as they once did, says Neil Maniar, director of the master of public health program, associate chair of the department of health sciences, and professor of public health practice at Northeastern.
“As we look at the numbers, it’s about responding as opposed to panicking,” Maniar says. “If we were seeing these numbers back in September of 2020, it would be a different story. But we’re in a very different place now.”

Alessandro Vespignani, Director of the Network Science Institute and Sternberg Family Distinguished University professor of physics, computer sciences, and health science at Northeastern University. Photo by Matthew Modoono/Northeastern University
In 2022, public health officials know a lot more about how to fight the virus. And that can begin with how we relate to the metrics.
“We need to think of cases differently and not compare the number that we have today with the numbers that we experienced in the past,” says Alessandro Vespignani, Sternberg Family Distinguished Professor and director of the Network Science Institute at Northeastern.
Record-high case counts might not be cause for concern in their own right because the omicron variant reportedly is less likely to cause severe illness than previous versions of the virus, particularly among fully vaccinated people and even more so among boosted people.
In the omicron-driven wave, “it’s not that the [case counts and hospitalization rates] are completely decoupled or divorced,” says Vespignani, who leads an infectious-disease-modeling team that projects future scenarios about the pandemic. “The two things now have a different proportionality factor.”
Earlier in the pandemic, case counts were an important indicator that things were getting worse because a certain percentage of cases were likely to end up in the hospital. Now, with omicron and vaccine protections, a much lower percentage of cases is likely to end up in the hospital.
But even if hospitalization rates represent a smaller proportion of case counts, if the sheer volume of case counts soars in the way that it has in this wave, Vespignani says, the raw number of hospitalizations can rise to alarming levels, too. And that’s exactly what is happening. As a result, many hospitals are short-staffed, having to cancel or delay nonemergency procedures, and some have called in the National Guard for support.
The vast majority of hospitalized coronavirus patients are unvaccinated, according to reports from across the country. The Philadelphia Inquirer reported Friday that 90% of COVID-19 patients at some hospitals in Pennsylvania were unvaccinated—and the percentage was even higher when it included people who were not fully vaccinated but had gotten one shot.

Neil Maniar, director of the Master of Public Health program, associate chair of the department of health sciences, and a professor of public health practice in the Bouvé College of Health Sciences at Northeastern University. Photo by Matthew Modoono/Northeastern University
There is utility for public health officials in continuing to monitor rising cases as a way of mapping the trajectory of the pandemic, says Vespignani. It can help healthcare systems plan ahead, as rising hospitalization rates tend to lag behind rising case counts.
But there are also reasons for individuals to continue to pay attention to COVID-19 cases. For one, every person who tests positive is someone who can isolate and prevent further spread, Maniar says. Even if you are vaccinated and your case is mild, the next person you encounter might not be vaccinated, might be immunocompromised, or might have a family member who is at high risk for a severe case.
Furthermore, “for an individual who is not vaccinated, [case counts] offer a good window into what their risk is,” Maniar says. “Being vaccinated may not necessarily prevent someone from getting it, but it will significantly reduce the likelihood that they will wind up in the hospital.”
Case counts, hospitalizations, and deaths aren’t the only metrics that can help indicate what the future of the pandemic might hold. Many municipalities are also detecting SARS-CoV-2, the coronavirus that causes COVID-19, in their area’s wastewater.
The levels of the coronavirus detected in wastewater samples can be an early warning sign for a surge in cases, Maniar says. Wastewater coronavirus recordings also have the potential to indicate when a wave of cases might be missed, as many mild or asymptomatic cases that go untested or unreported from at-home tests might not be making it into the official counts.
Despite setting records in the current omicron-fueled wave of cases and hospitalizations, a lot has changed since the beginning of the pandemic.
A big part of why things are different in 2022, Maniar says, is vaccines and booster shots. One year ago, vaccines were just beginning to become available to the most at-risk people. But now, everyone over the age of 5 is eligible to receive the shots in the U.S.
For families with children in the younger age group or immunocompromised individuals, things are still tricky, Maniar says, “and that’s why it’s really important that we deploy our tools that we have available to the fullest extent possible when we see these kinds of case numbers.”
“Early in the pandemic, we only had a few tools in our toolkit to respond to the pandemic. We now have multiple tools,” he says. There are the non-pharmaceutical interventions of social distancing, mask-wearing, and other precautions. There are also a selection of testing approaches to be able to make informed decisions about your exposure and potential to expose others. And there are several different COVID-19 treatments coming to the table, including antiviral pills that could help keep more severe cases and at-risk individuals out of the hospital. And, of course, there are vaccines that reduce the risk of a coronavirus infection becoming severe.
“The pandemic is going on for longer than anybody hoped,” Maniar says, adding that history shows us that pandemics take a while to beat back. But he also suggests looking back to the early days of the pandemic as a lens into what we have been able to learn and achieve in less than two years.
“Throughout this pandemic, we’ve gotten a better sense of how to deploy the tools that we have in the best way possible and the effectiveness of those tools,” he says. “By April of 2020, we knew masks were really important. But back then we also thought that we had to wipe down all of our groceries. We’ve now learned that you’re not going to die if you forgot to sanitize a loaf of bread. But we have also learned that wearing a mask is an incredible way to protect yourself and protect others from getting COVID.”
For media inquiries, please contact Shannon Nargi at s.nargi@northeastern.edu or 617-373-5718.





