What is your fascia? And why wellness is connected to the body’s underappreciated connective tissue
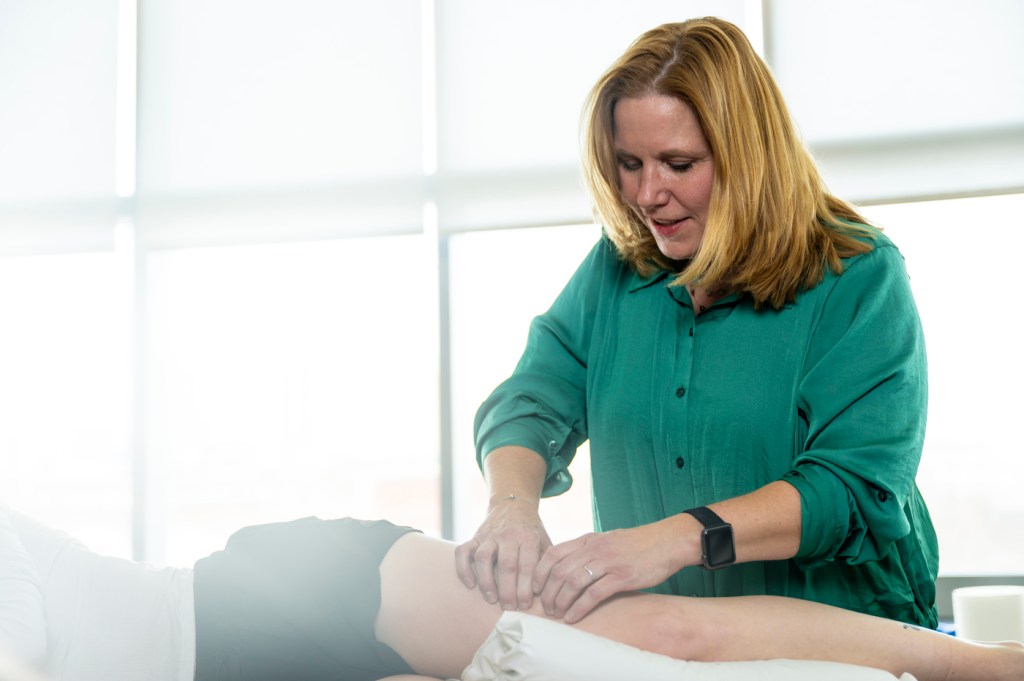
If you’re in pain or experiencing pain or limited mobility, you may suspect a problem with your muscles or joints.
What if the problem lies elsewhere, in your fascia?
Health practitioners including physical therapists, chiropractors and massage therapists increasingly are paying therapeutic attention to this long-overlooked part of the bodily system.
As well they should, says Maureen Watkins, associate clinical professor in Northeastern’s Department of Physical Therapy, Movement and Rehabilitation Sciences.
“Fascia is basically a thin layer of connective tissue that separates muscles and organs from other structures” and keeps things moving smoothly by reducing internal friction, says Watkins, who holds both physical therapy and massage licenses.
Like a stocking, it engulfs the entire body and dynamically stabilizes it, she says.
“It’s everywhere doing everything. It’s vital for our mobility, our stability, our movement,” says Scott Diamond, a chiropractor in Boston who holds a degree from Northeastern.
Injuries to the fascia from accidents, poor posture and even stress can turn the supple tissue hard, Diamond says. “It feels stuck, like a 2-by-4 versus a wet sponge.”
An injury or damage to one part of the fascia can affect the fascia in a different part of the body, Diamond says.
“A lot of time in the human body we see compensatory patterns that are producing pain,” he says. “Your shoulder hurts, but it could be driven by your right hip being tight.”
The results can be chronic pain and limits to mobility that can only be relieved through therapies targeted to restoring the fascia, such as a process called myofascial release, Watkins says.

Why fascia has been underappreciated
Treating damaged or injured fascia started gaining popularity about seven to 10 years ago with a technique called structural integration that was the next generation of fascia therapy developed by pioneer practitioner Ida Rolf, who died in 1979, Diamond says.
And it’s only been in the last several years that treating fascia has gained respect in mainstream medicine, he says.
It’s not because fascia is invisible.
Cutting up cadavers in chiropractic school, the webby tissue — the same thing cooks handle when they separate chicken breast from skin — was discarded without further study, Diamond says.
“We would move this tissue out of the way to see other things. It was viewed as body filler, almost like the packing you would see in an Amazon box,” he says.
It didn’t help that for years there were no technical tools such as X-rays to view injuries to fascia, Watkins says.
She says that the situation is now changing with the development of musculoskeletal ultrasound, during which probes can be applied to the skin to see adhesions, scar tissues and thickness asymmetries in the fascia underneath.
She assesses patients’ fascia health the old-fashioned way — by using her hands to feel invisible scarring and whether the fascia is hardened or flexible and able to slide or glide over muscles, organs and bone.
Featured Posts
‘You’re not stuck’
The good news is that people who suffer fascial pain, even for years, can get relief through a combination of therapeutic techniques and their own focused movement.
“You can change the way the fascial system works,” Diamond says. “You’re not stuck.”
Watkins says she used myofascial release to treat a patient who suffered limited mobility and a profound lack of strength 20 years after a car accident.
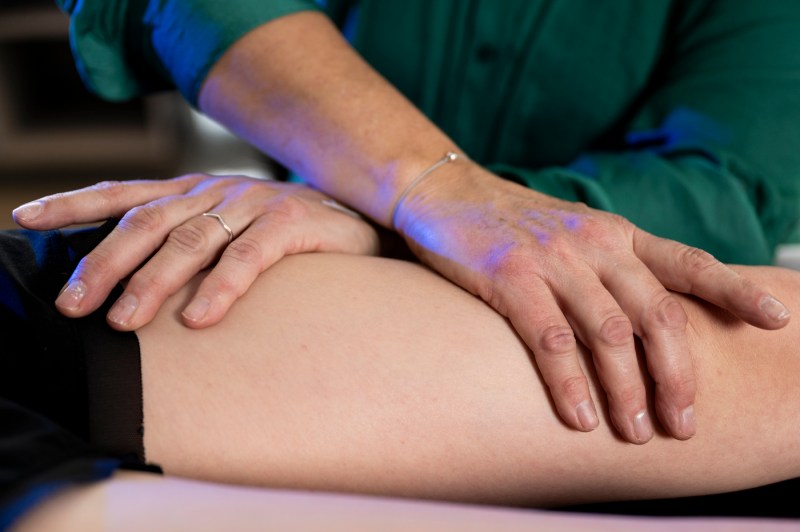
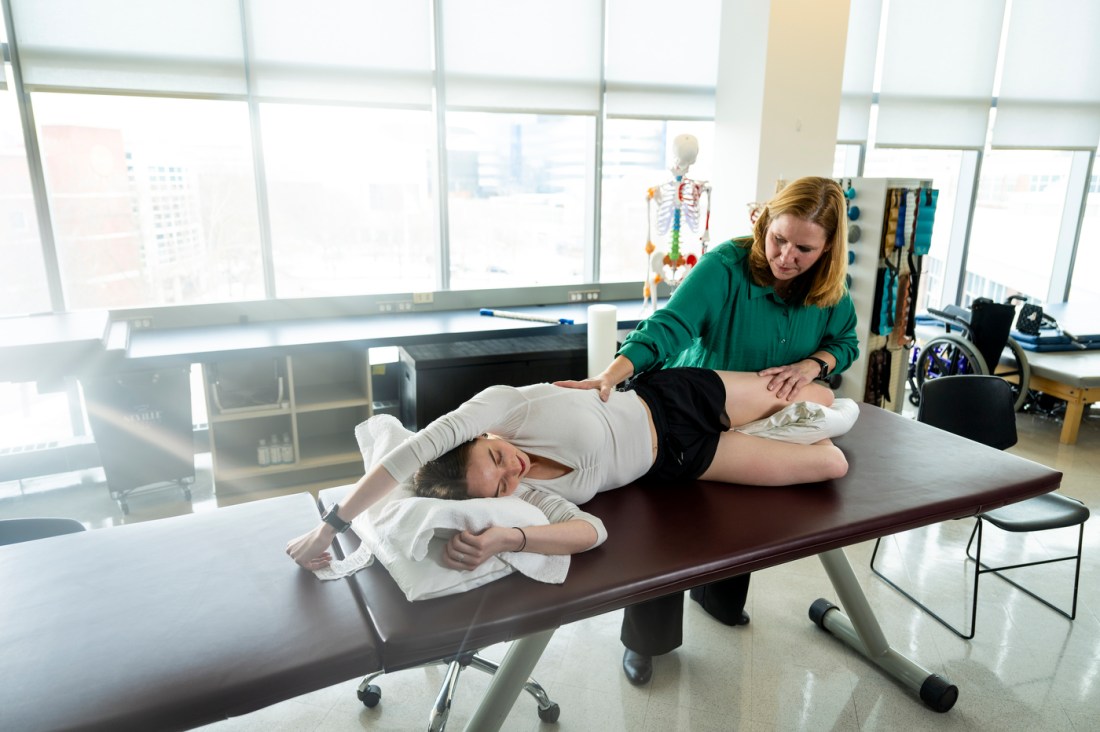
“Myofascial soft tissue work involves applying a sustained pressure on targeted areas of the body where fascia may be restricted,” Watkins says.
“This pressure helps to release the restriction in the tissue which will result in improved range of motion, less pain and improved function,” she says.
“Typically, during myofascial release, I will maintain pressure for approximately three to five minutes at a time in the targeted area. Using steady pressure is the key,” Watkins says.
“Fascia fibers are slow to respond to pressure and they need sufficient time to soften and elongate. I then follow up with an active range of motion plan and a functional activity to help the patient improve and meet their goals.”
As the automobile crash patient’s fascia responded and her stability improved, the woman who was unable to lift weights — or even get a massage — without collapsing in pain was able to work out again and rediscover life without pain, Watkins says.
Diamond says unlike during regular massages, his myofascial treatments incorporate patient movement during the procedure, for instance having them move their feet while he works on calf tissue.
The key to a soft supple fascial system is movement — purposeful, mindful movement, Diamond says. Consistent treatment and movement are like adding water to dried ramen noodles. “The fascia starts to move.”

How do you know it’s your fascia?
Chronic, lingering pain that is not resolved by therapy that addresses the muscles and joints could point to fascia involvement, Diamond says.
“You just can’t seem to get over the hump,” he says. “You say, ‘I hurt my shoulder and I keep treating it and treating it but it doesn’t seem to get better.’”
Watkins says the education and training physical therapists receive helps them to determine what is muscle pain versus joint or fascial pain and how they are all related. “It’s one-stop shopping,” she says.
Out-of-pocket sessions with practitioners of structural integration technique can be pricey, costing clients $200 to $300 for 90 minutes to two hours, Diamond says.
In most cases, health insurance will cover physical therapy and chiropractic treatment that addresses fascia, he says.
“A good question to ask (the practitioner) is have you had any training in myofascial technique?” Diamond says.
You can help your fascia every day
After an injury to the fascial system, regular movement, stretching and self-treatment should be a daily practice since fascial restrictions can take one to two years to be fully restored to their previous state, Watkins says.
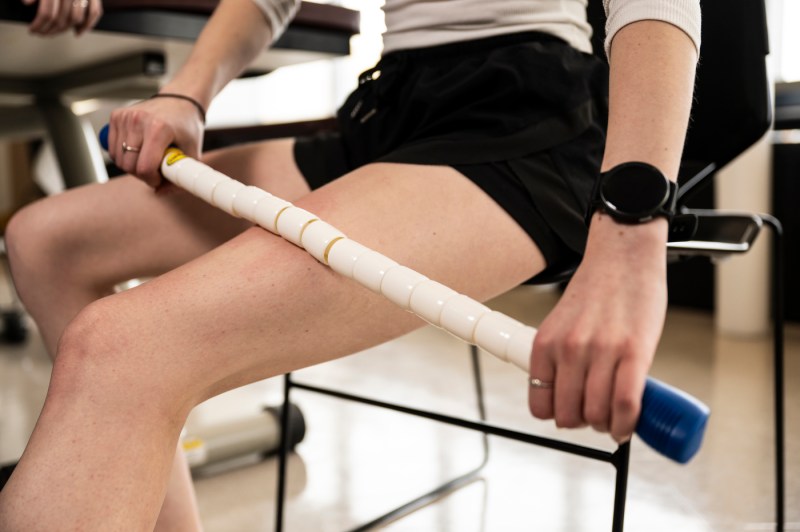
“Individuals can also perform self-myofascial massage through the use of foam rollers, massage sticks and balls with guidance from a physical therapist,” she says.
Daily walks and deep breathing from the diaphragm go a long way to maintain healthy fascia, as does adequate water intake, Watkins says.
Diamond says proper breathing through the nose is more important than people realize. He advises people to only breathe through their mouth when they are talking.
Anything else puts stress on the body by delivering less oxygen — and that can impact the fascia, Diamond says.
Good posture is also an important part of keeping fascia elongated, as will hanging from a pullup bar or doorframe, he says.
“Fascia responds well to a range of motion,” Diamond says.
So let your childlike self emerge and view the world as a jungle gym, he says.
When you’re making coffee, put your hands on the counter, spread your knees and lean into the counter. Swing your arms and rotate them as though you are a water sprinkler, Diamond says.
Your fascia, he says, will thank you.











