New RSV immunization approved by FDA. Why it’s ‘an important development in pediatric medicine’
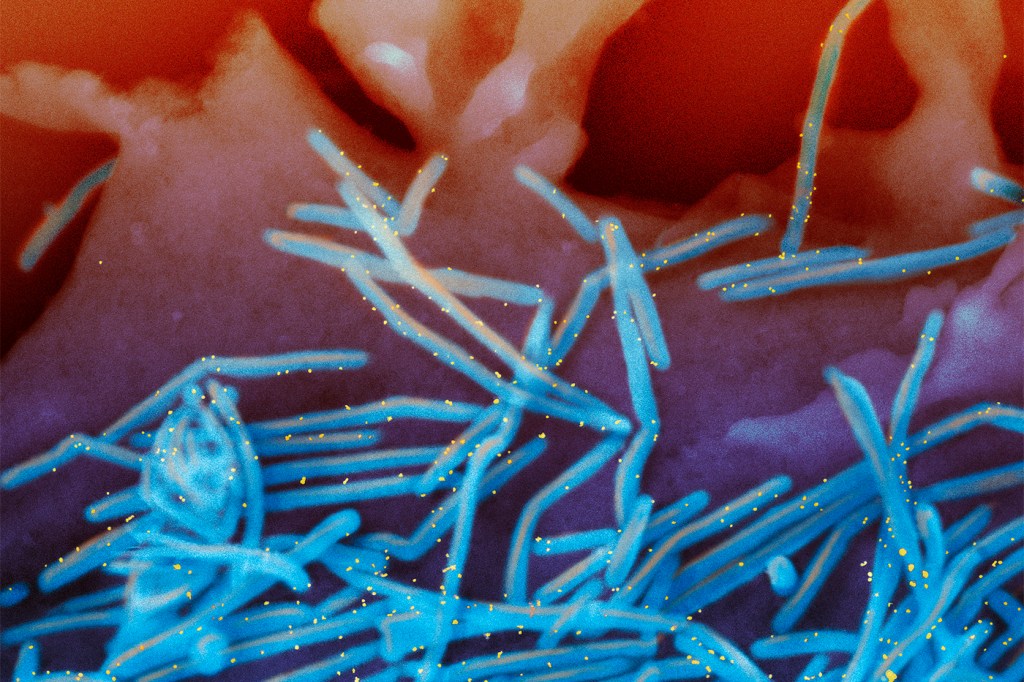
For many parents and babies, this past winter was a rough time as an early flu season combined with RSV (respiratory syncytial virus) and COVID-19 to create a “tripledemic” of infectious respiratory illnesses.
This coming winter could spell relief from infant RSV.

This week, the FDA approved a monoclonal antibody treatment to protect infants and young babies against RSV, which the American Academy of Pediatrics says results in the hospitalization of approximately 1 to 3% of children under 12 months of age every year.
Nirsevimab, the antibody which will be marketed by AstraZeneca and Sanofi as Beyfortus, will be given in one shot to children born during or just entering their first RSV season, according to a press release from the FDA.
The shots also will be available for children up to 24 months of age who remain vulnerable through their second RSV season due to medical conditions.
“It’s such an important development in pediatric medicine,” says Neil Maniar, director of Northeastern’s public health program. “RSV is one of the leading causes of hospitalization for infants. This is the first time we have a treatment available for all infants.”
What is RSV?
RSV is a lower-respiratory tract disease that typically starts showing up in babies in the fall with cases continuing to crowd doctors’ offices until spring.
“There is a high degree of seasonality to RSV,” Maniar says.
This past winter, the confluence of early flu, COVID-19 and a spike in RSV cases was “one of the things we were very concerned about,” he says.
The plan is for Beyfortus to be administered in the hospital to infants born during peak season and to children born before the season.
“It’s a really important opportunity to protect infants during this peak season,” Maniar says.
Before Beyfortus is available in pediatricians’ offices, it needs to be formally approved by the CDC’s Advisory Committee on Immunization Practices, which is expected to take place at ACIP’s next meeting scheduled for Aug. 3.
Health-education campaign
A rollout is expected by fall.
“We need to make sure that this is coupled with a health-communication and health-education campaign to make individuals understand why this is important and how it is different from a vaccine,” Maniar says. “This is not a vaccination, but it is immunization.
“A vaccine causes antibody production in the body,” he says. “This is a passive immunization. You are administering the antibody directly. The antibodies are what will attack the virus. You do not need the infants’ immune system to respond.”
The result, he says, is “a much higher likelihood of success in treatment.”
The FDA says nirsevimab, or Beyfortus, reduced the risk of RSV in two trials by 70% and 75% in infants who had received the immunization versus those who received the placebo.
The third trial, in children up to 24 months of age who remain vulnerable to RSV complications, “provided evidence for the use of Beyfortus,” according to the FDA.
Premature babies already protected
With CDC approval, nirsevimab, or Beyfortus, will be the second antibody available to protect babies and young children against RSV.
Already in use is palivizumab, marketed as Synagis, which protects premature babies who are younger than 6 months from RSV.
Synagis “has to be given more frequently. It’s not something that was really designed for the general population of newborns,” Maniar says. “The new monoclonal antibody treatment is a single injection that lasts for five months.”
Also before the FDA for consideration is a vaccine for pregnant women that would protect babies against RSV.
“The maternal-to-fetal transmission of protection is really important,” Maniar says. “If you have the opportunity to pass antibodies from the mother to the fetus, the moment the infant is born it will have protection against RSV.”
Vaccine protects older people
Older people also are susceptible to complications from RSV. In May, the FDA approved Arexvy, the first vaccine against RSV, to protect people ages 60 and older.
Maniar says he wants to see the rollout of Beyfortus coupled with a “transparent education and communication campaign” as well as widespread accessibility.
The CDC says up to 80,000 children under 5 years of age are hospitalized every year with RSV, and Maniar says it causes about 300 deaths a year.
“RSV is very common,” he says. “Typically most individuals in their first year of life are exposed to it. But 50 percent hospitalizations are among otherwise healthy newborns, not those who fall into the most vulnerable category. RSV is a serious illness.”
Cynthia McCormick Hibbert is a Northeastern Global News reporter. Email her at c.hibbert@northeastern.edu or contact her on Twitter @HibbertCynthia.






