Should I mix and match my COVID-19 booster shot?
As concerns about the omicron variant mount, federal public health officials have strengthened their stance on booster shots for COVID-19 vaccines.
On Monday, U.S. Centers for Disease Control and Prevention issued a recommendation that everyone ages 18 and older get a booster shot six months after their second injection of one of the mRNA vaccines, or two months after the single-dose Johnson & Johnson vaccine.
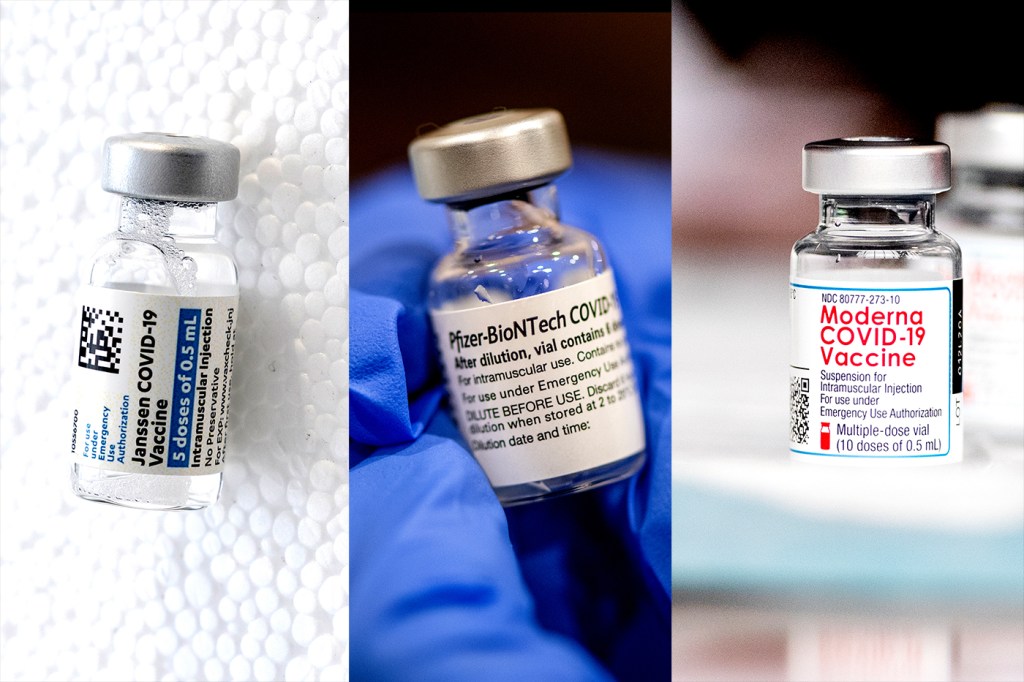
As adults go to get their booster shots, they may face a choice. The CDC has said that it is safe for people to get a booster shot that is different from the vaccines they originally received. In this “mix and match” approach, someone who received two Pfizer-BioNTech shots in their initial vaccination series might opt to get a Moderna booster shot, for example.
The option to mix and match dosing for booster shots has caused a lot of confusion for vaccine-seekers. It offers nine different combinations of vaccines, depending on what you started with. The main question: Is any particular combination better than the others?

Brandon Dionne, associate clinical professor of pharmacy and health systems sciences at Northeastern. Photo by Matthew Modoono/Northeastern University
When the National Institutes of Health examined the safety and efficacy of a mix and match approach to booster shots, their results suggested that the immunity of people who got the single-shot J&J vaccine would be best boosted by one of the mRNA booster shots (Moderna and Pfizer-BioNTech). The differences between those two, however, were subtle.
Most public health experts agree that those distinctions are probably insignificantly small, and they say that the best shot is the shot you can get most easily.
“Any additional dose, regardless of what you got initially, is going to increase your immune response and provide more protection,” says Brandon Dionne, associate clinical professor of pharmacy and health systems sciences at Northeastern. “It’s all going to increase your antibody response.”
But for those who can and want to choose, the NIH study offered some insights.
The study included 458 people, and tested and compared the antibody levels in every one of the nine possible combinations of vaccines and boosters. That meant that the groups representing each of the combinations were notably small (about 50 participants). But, says Mansoor Amiji, university distinguished professor of pharmaceutical sciences and chemical engineering at Northeastern, “it was a reasonable study, and any study that informs decision-making is always helpful.”
“It was quite startling to see the results,” he adds.

Mansoor Amiji, university distinguished professor of pharmaceutical sciences and chemical engineering at Northeastern. Photo by Matthew Modoono/Northeastern University
The evidence toward the mRNA boosters was clear. Two weeks after a booster shot, people who had initially gotten a J&J shot and followed it with a Moderna booster had average antibody levels that were 9.8 times higher than those who had gotten two J&J shots. Those who got a Pfizer-BioNTech booster were close behind.
Still, there’s no bad option. In another study from earlier this year, which used 30,000 participants, a second J&J shot boosted efficacy to 94% protection against mild to severe cases of COVID-19.
As for the mRNA combinations, the volunteers who had received three doses of Moderna had the highest antibody levels found in the study. Participants who got a Moderna booster after the two-dose Pfizer-BioNTech series ranked a close second. Those who started with Moderna and boosted with Pfizer-BioNTech had the third highest antibody levels.
Moderna seems like a clear winner, right? Not so fast.
That NIH study used a full dose of the Moderna shot, but an advisory committee to the U.S. Food and Drug Administration has recommended that Moderna booster shots be a half-dose. However, a half dose might be plenty, Dionne says.
“The original Moderna dose was 100 micrograms. The Pfizer dose was 30 micrograms,” he says. “So the Moderna booster is a half dose at 50 micrograms, but that’s still more than the full dose Pfizer. I don’t think anyone really knows exactly what that means, though.”
Another wrinkle: Scientists aren’t sure exactly how important those slight differences in antibody levels and dose amounts are in the real world.
“The threshold [of antibody levels] that you need in order to get continuous protection is dependent on a number of factors,” Amiji says. For example, if you spend a lot of time indoors in a crowded area, if you are exposed to SARS-CoV-2, the coronavirus that causes COVID-19, the viral load that hits you would likely be a lot higher than if you were outdoors when you were exposed. “The threshold of protection that you need varies person to person.”
Furthermore, antibody levels are not the only way the vaccines offer immunity to the virus. There’s also a cellular response, Amiji says. “That basically arms the body by giving a sufficient amount of information to an immune cell saying, if you see a cell that’s infected with the virus, just go and destroy that.”
For some, efficacy might not be the most important metric in choosing a booster, Dionne adds. There might be risk factors that are specific to you that might make you shy away from one particular vaccine, he says. For example, with the mRNA vaccines, in younger men there is a slightly increased risk of myocarditis, an inflammation of the heart. Or, there were reports of an extremely rare brain clot in premenopausal women who had gotten the J&J vaccine. Dionne emphasized that those risks are still incredibly low, but anyone concerned about severe side effects should speak to their doctors.
Other side effects could sway some patients to stick to their original vaccine types, or to mix it up, Dionne says. If you had a strong reaction to your first shots, or shot, you might opt to try a different one this time around.
“There’s not really a right or wrong answer,” Dionne says, suggesting that convenience might be more important for some. “Whatever you can get is probably the right one for you.”
For media inquiries, please contact Marirose Sartoretto at m.sartoretto@northeastern.edu or 617-373-5718.





